Why Do Moms Choose Us?
Lactation Link is a group of International Board Certified Lactation Consultants (IBCLCs) that are all about ‘Creating Confident Families’ when it comes to breastfeeding & pumping! Our network is a leading provider of educational resources, online prep courses and individualized support that empowers new moms to reach their breastfeeding goals.
Explore Our Top Courses


Breastfeeding Basics
Learn all about breastfeeding, right from the comfort of your own home. This 70-minute course will transform you from unsure to radiantly confident in your breastfeeding abilities. You will learn everything you need to know, from what to do for your first feeding to finding breastfeeding support in your community.
Learn More
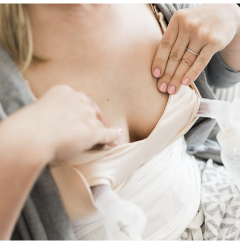
Pumping & Storing
This is a must-have course for all moms wanting to learn how to maximize milk expression and the safe handling of breastmilk. This 45-min course will give you all the know-how for pumping and storing breastmilk, and everything you need to organize, schedule, and establish your pumping goals.
Learn More

Breastfeeding Hurdles & How-To’s
Do you want to know how to prepare for the hurdles all breastfeeding moms experience? Then this course is perfect for you! This 60-minute course will empower you to breastfeed with optimal health for you and your baby. Includes introducing solids and options for weaning.
Learn More

"Your course and support community were instrumental in my two-year nursing journey! Thank you!”
–Marley Sessa, Google Reviews
As Seen In